Predictive Analytics in Cardiology: From Risk Stratification to Prevention
Predictive analytics in cardiology uses historical patient data, statistical models, and AI to forecast cardiovascular risks before symptoms appear. By identifying high-risk patients earlier, it enables clinicians to shift from reactive treatment to proactive prevention—improving outcomes while reducing avoidable hospitalizations.
This continuous algorithmic oversight grants clinical leadership absolute visibility into emerging patient risks. By rigorously analyzing historical patterns and live operational signals, these platforms empower teams to pinpoint the exact populations requiring immediate medical intervention.
Executing this proactive strategy permanently reallocates critical facility resources toward targeted early prevention. Rather than playing catch-up as patients’ conditions deteriorate, today’s heart health initiatives use foresight to consistently place at-risk individuals at the forefront, effortlessly bridging preventative medical action with sustainable clinical patient health outcomes.
What Predictive Analytics Means in Cardiology?
In cardiology, predictive analytics refers to the use of clinical data, machine learning models, and statistical techniques to predict future cardiovascular events such as heart failure, coronary artery disease, or hospital readmissions.
Predictive healthcare analytics turns clinical data into accurate forecasts for upcoming heart events. This approach changes service lines from reactive to proactive care.
Data Sources Used in Cardiology Analytics
Cardiology predictive models continuously ingest data from the following comprehensive data streams:
- Electronic patient health records
- Advanced imaging data (e.g., echocardiograms, CT scans)
- Laboratory results
- Wearable and remote monitoring data
Predictive Models in Healthcare
Advanced algorithms process historical data patterns to generate exact risk scores. These models predict readmissions and isolate acute disease progression.
Risk Stratification Techniques
Strict algorithmic stratification categorizes patient populations by absolute event probability. This clear visibility helps clinical leaders focus on important interventions. It also allows them to optimize resource allocation in specialized facilities.
The Role of Risk Stratification in Cardiovascular Care
Executing strict cardiology risk stratification dictates the operational value of predictive analytics. These models pinpoint specific patient populations at risk of imminent clinical deterioration, severe complications, or avoidable facility use. This forces clinical leadership to prioritize high-acuity interventions effectively.
In practice, clinicians often combine traditional cardiovascular risk scoring models such as ASCVD or Framingham—with predictive analytics to enhance accuracy and personalize risk assessment at the patient level.
In cardiovascular services, this visibility focuses on specific patients. It includes people with acute heart failure. It also includes those with worsening coronary artery disease. Lastly, it covers those at risk of going back to the hospital. Exposing these vulnerabilities leads to quick clinical actions. This includes better care coordination, faster follow-ups, and strict changes to protocols.
Precision cardiovascular risk scoring directly governs chronic disease management. Algorithmic stratification dictates exact resource allocation, concentrating specialized clinical effort exclusively on the highest-risk heart failure and hypertensive cohorts to maximize programmatic impact and eliminate wasted administrative effort.
Operating under strict facility capacity constraints demands targeted patient management. Predictive risk modeling permanently replaces broad, manual monitoring by isolating the exact individuals requiring immediate early intervention, aligning limited clinical resources directly with maximum patient outcomes.
Key Data Inputs Used in Cardiology Predictive Models
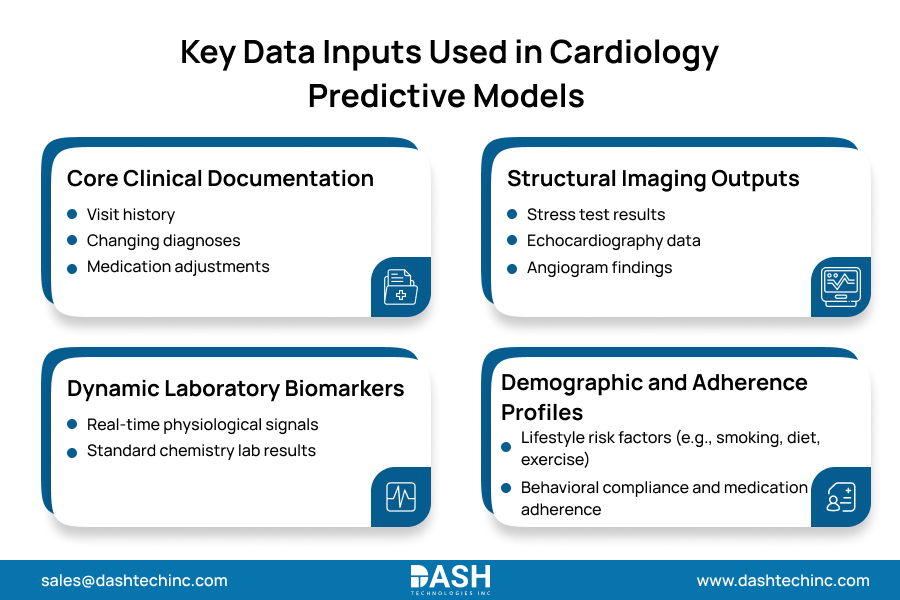
Effective cardiology of patient data analytics needs to integrate many fragmented data sources. This helps create a single, high-quality patient profile. Fragmented data structures don’t work well. To create useful cardiovascular predictions, we need a complete, multi-dimensional input strategy.
Service-line executives must mandate the continuous integration of four core data streams:
- Core Clinical Documentation: Visit history, shift diagnoses, and active medication adjustments.
- Structural Imaging Outputs: Data extracted from stress tests, echocardiography, and angiograms.
- Dynamic Laboratory Biomarkers: Real-time physiological signals and standard chemistry results.
- Demographic and Adherence Profiles: Lifestyle risk factors and documented behavioral compliance.
Cardiovascular risk is never one-dimensional. A patient’s clinical trajectory is simultaneously dictated by disease severity, supply chain utilization, and social context. Aggregating these disparate sources eliminates the blind spots of single-variable analysis, directly increasing predictive accuracy and allowing clinicians to intervene with absolute confidence in the patient’s actual risk profile.
How Predictive Analytics Supports Preventive Cardiology?
Achieving clinical excellence demands utilizing preventive cardiology analytics to intercept disease upstream. Advanced predictive algorithms instantly process subtle clinical signals to dictate early intervention long before acute hospitalization or emergency presentation occurs.
This proactive infrastructure drives three core operational mandates for absolute cardiovascular disease prevention:
- Early detection of escalating risk by continuously aggregating diagnostic data and historical utilization trends.
- Proactive monitoring across expensive chronic populations, permanently eliminating manual surveillance inefficiencies.
- Personalized treatment pathways, ensuring premium clinical resources are deployed exclusively based on absolute patient risk rather than broad protocols.
Deploying these advanced models requires a zero additional administrative burden. Algorithmic surveillance runs continuously in the background. It equips clinical teams with prioritized patient queues. It also provides exact risk stratification. Additionally, it offers clear guidance on taking immediate medical action.
Let’s Redefine Prevention in Cardiology
Turn predictive intelligence into meaningful care! Help your teams act earlier, decide smarter, and deliver better outcomes.
Talk to Our ExpertsOperational Benefits of Predictive Analytics for Cardiology Departments
Deploying cardiology operational analytics fundamentally transforms how facility leaders strictly govern limited specialized resources. Executing predictive healthcare operations completely eliminates reactive capacity management and standardized patient workflows. This algorithmic oversight dictates three core facility advantages:
- Precision population management, stratifying patient groups by absolute clinical risk to dictate targeted follow-up strategies.
- Strict resource allocation, forcing clinics and inpatient care coordinators to concentrate time exclusively on patients presenting the highest predicted clinical need.
- Aggressive readmission reduction, utilizing advanced models to isolate vulnerable populations immediately after discharge for early medication review and transition support.
This targeted visibility guarantees optimal procedural planning. By directing clinical bandwidth toward genuine risk, cardiovascular departments maximize overall service line efficiency and permanently eliminate avoidable facility utilization entirely.
Explore how optimizing cath lab utilization can further enhance efficiency and resource allocation across cardiology departments.
Technology Platforms Supporting Predictive Cardiology Analytics
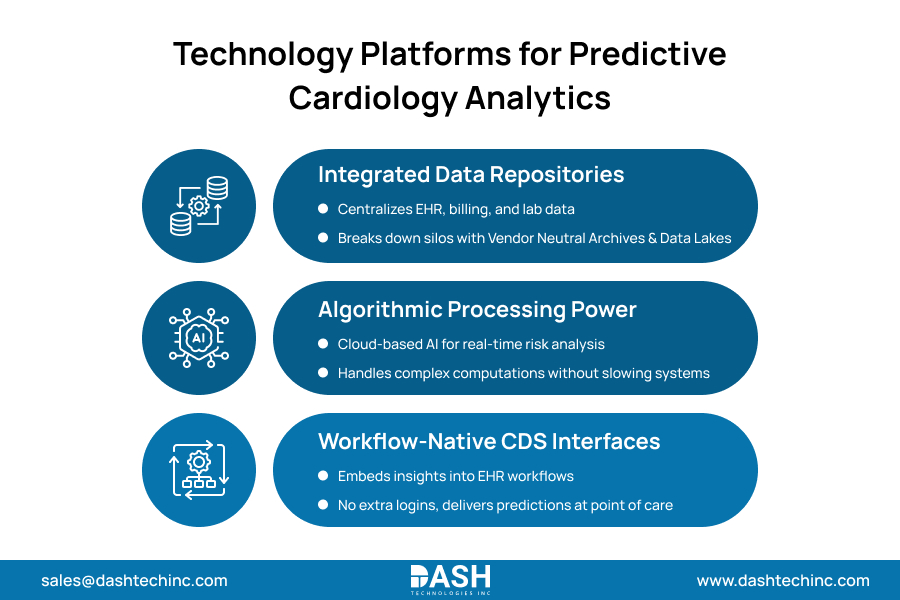
Building scalable predictive capabilities demands rigorous investment in enterprise cardiology analytics platforms. Modern AI in cardiology analytics enables real-time cardiovascular risk prediction by combining scalable computing infrastructure with advanced predictive healthcare analytics tools. The modern infrastructure of healthcare predictive analytics tools requires three interconnected technological layers to execute seamlessly:
- Integrated Data Repositories: Vendor Neutral Archives and Advanced data lakes aggressively break down legacy departmental silos, forcing the continuous synchronization of EHR, billing, and catheterization lab inputs into one centralized foundation.
- Algorithmic Processing Power: Cloud-native AI engines process complex risk variables continuously. This dedicated infrastructure executes heavy predictive computations without compromising the speed of primary facility servers.
- Integrated Clinical Decision Support (CDS): This terminal interface injects algorithmic foresight directly into the physician’s native workflow. By triggering actionable, in-chart alerts, CDS eliminates the operational friction of secondary applications and drives immediate clinical execution.
Challenges in Implementing Predictive Analytics in Cardiology
Despite its potential, implementing predictive analytics in cardiology comes with several challenges:
- Fragmented healthcare data: Patient data often exists across multiple systems, making integration complex
- Model accuracy and bias: Predictive models must be validated to avoid inaccurate or biased outcomes
- Clinical adoption barriers: Physicians may hesitate to trust or rely on algorithm-driven insights
- Integration with workflows: Embedding analytics into existing clinical systems without disruption can be difficult
Addressing these challenges requires a strong data foundation, continuous model validation, and alignment with clinical workflows.
Best Practices for Implementing Predictive Analytics in Cardiology Programs
A strong predictive healthcare strategy starts with integration, not just modeling. Cardiology analytics implementation works best when predictive efforts are tied to specific clinical and operational goals.
Administrators must mandate four rigorous deployment standards:
- Integrate comprehensive clinical and operational data to establish absolute contextual accuracy.
- Validate algorithmic models against local patient populations and facility workflows, explicitly rejecting generic external assumptions.
- Embed predictive insights natively into existing clinical workflows, driving immediate medical action without generating additional administrative friction.
- Mandate continuous performance monitoring, rigorously refining algorithmic accuracy, and operational usability over time.
Treating predictive infrastructure as a one-time IT project guarantees failure. Best cardiovascular programs continuously calibrate their models, ensuring algorithmic foresight directly dictates measurable improvements in patient care delivery.
Conclusion
Securing profitability in the future of cardiology analytics demands treating algorithmic foresight as foundational facility infrastructure rather than an isolated technology pilot. Deploying rigorous predictive cardiology models forces the complete abandonment of reactive, episodic treatment in favor of high-velocity proactive prevention. This permanent operational shift directly maximizes clinical patient outcomes while strictly enforcing sustainable financial performance.
Attempting to manage complex cardiovascular populations through late-stage medical intervention actively destroys service line margins. Market-leading facilities dictate success by leveraging advanced risk stratification and proactive clinical pathways to intercept disease progression early. Executing this data-driven transition guarantees compounding ROI through drastically reduced readmissions, optimized specialized labor allocation, and absolute dominance in value-based reimbursement contracts.
Ready to improve cardiovascular outcomes and reduce readmissions with predictive analytics? Get in touch with our team to explore how a customized approach can work for your cardiology programs.
Frequently Asked Questions
About Dash

Dash Technologies Inc.
We’re technology experts with a passion for bringing concepts to life. By leveraging a unique, consultative process and an agile development approach, we translate business challenges into technology solutions Get in touch.