From Cath Lab to Follow-Up Closing Data Gaps in Cardiology Workflows
Cardiology workflow optimization begins with understanding where care transitions break. In most cardiology programs, the workflow doesn’t fail inside the cath lab or clinic. It fails in the space between them, where communication and processes can break down. Data gaps in healthcare show up at every handoff; this includes diagnostics, intervention, recovery, and follow-up. When teams delay or share incomplete information, they lose visibility. This can cause patients to fall through the cracks.
The most critical failures in cardiology workflows don’t occur during procedures when they occur during transitions between diagnostics, intervention, discharge, and follow-up.
For a deeper look at how analytics strengthens modern cardiology programs, explore our guide on The Role of Data Analytics in Modern Cardiology Care Delivery.
Modern cardiology care delivery spans multiple settings and teams. Each transition brings risks. These include data loss, communication delays, and missed chances for help. Closing these gaps improves outcomes. It strengthens care coordination and reduces operational strain. Best of all, it does this without adding new administrative burdens.
Understanding the End-to-End Cardiology Care Workflow
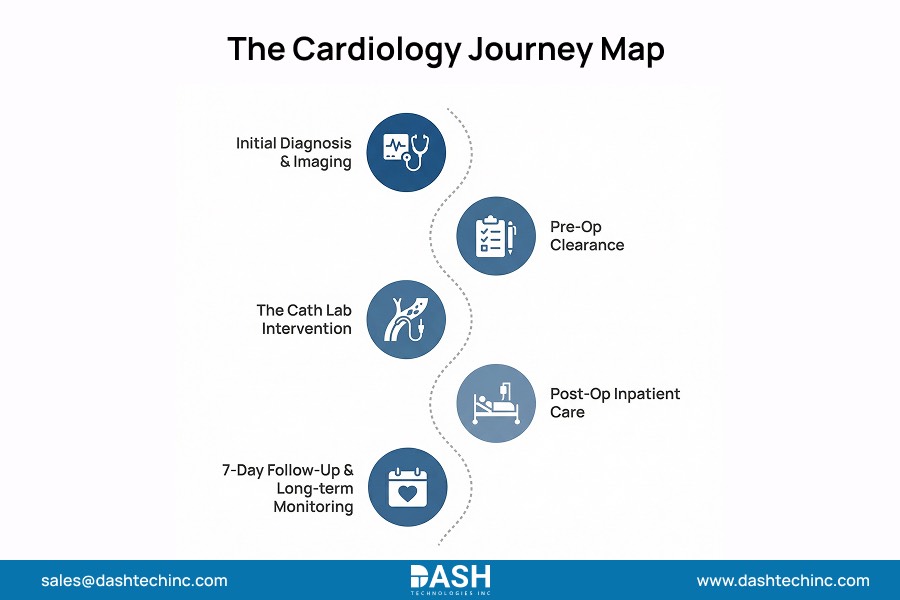
Cardiology care workflows cover a wide range. Each step produces important clinical data. Data must move seamlessly across systems to enable cardiology workflow optimization.
- Pre-Procedure Evaluation
The end-to-end cardiology workflow begins with the aggregation of history, physicals, and diagnostic imaging (ECG, Echo, Stress tests) to determine the necessity of intervention. - Cath Lab and Intervention
Procedural details and hemodynamics are key. Device info, complications, and post-procedure orders are the “source of truth.” They determine what happens next in healthcare workflow analytics. - Inpatient Recovery and Discharge
Vitals, complications, meds reconciliation, and discharge instructions bridge inpatient to outpatient. Missing data here leads to redundant work or gaps. - Outpatient Follow-Up and Monitoring
Post-discharge visits, remote monitoring, & medication titration help track long-term outcomes. This continuity helps find problems early. This includes stent thrombosis and heart failure decompensation.
Where Cardiology Data Gaps Commonly Occur in Workflows
Despite advanced technology, fragmented cardiology workflows remain common. Breakdowns typically occur at transition points, highlighting the critical need for cardiology workflow optimization.
Between Diagnostics and the Cath Lab
- Imaging and test results stored in separate systems
- Referral information missing or incomplete
- Scheduling delays due to limited data visibility
During Post-Procedure Transitions
- Procedural notes not immediately available to recovery teams
- Medication updates delayed or unclear
- Limited visibility into discharge planning
Between Discharge and Follow-Up Care
- Missed follow-up appointments
- Lack of communication with primary care providers
- Limited tracking of patient adherence and outcomes
These breakdowns are predictable and preventable.
The Clinical and Operational Impact of Cardiology Data Gaps
Gaps don’t just affect patients; they create operational inefficiencies cardiology-wide. When cardiology care coordination relies on incomplete handoffs, the result is both clinical risk and operational drag.
Common impacts include:
- Delayed follow-ups: Patients can slip through the cracks. This often happens when a follow-up step isn’t scheduled or confirmed.
- Redundant tests: When lab results aren’t available during a care transition, it’s easier just to reorder the test. This wastes time and resources.
- Missed risk signals: Post-procedure warnings, abnormal lab results, or symptom patterns aren’t escalated in a timely manner.
- Increased clinician workload: Teams spend time on “detective work”—calls, chart hunting, and re-documenting information.
This is where healthcare workflow analytics becomes essential: you can’t fix what you can’t see, and you can’t sustain improvements if the burden stays manual.
Optimize Your Cardiology Workflows
Explore how integrated analytics can close data gaps and improve care continuity across the cardiology journey.
Explore Cardiology AnalyticsWhy Manual Processes Can’t Close Cardiology Workflow Gaps
Manual healthcare workflows→phone calls, spreadsheets, inbox reminders, and memory; can temporarily patch holes, but they don’t scale. They also increase cardiology documentation burden and create inconsistent handoffs across shifts, sites, and teams.
Manual approaches fail because:
- They depend on individual vigilance instead of system reliability.
- They lack consistent accountability; no one can easily tell where a handoff broke.
- They create parallel workflows outside core systems, increasing cognitive load and time.
Many cardiology leaders are already exploring structured approaches to reduce documentation strain, as discussed in How Cardiology Providers Can Improve Outcomes Without Increasing Clinical Burden.
How Data Integration Improves Cardiology Workflow Continuity
The solution lies in cardiology data integration. By making interoperable healthcare systems the standard, data becomes a utility that follows the patient.
- Input: Procedural data from the cath lab hemodynamics system.
- Integration: Real-time push of that data into the central hospital EHR.
- Outcome: Immediate visibility for recovery teams and outpatient clinics, enabling proactive care.
This “unified view” makes sure the doctor in the clinic and the surgeon in the lab see the same data. This cuts out guesswork and provides a better care coordination reliability.
Using Analytics to Monitor and Optimize Cardiology Workflows
Cardiology workflow analytics (healthcare process analytics) turns continuity into something measurable. Instead of only tracking volumes (number of procedures), leaders can track flow (how reliably patients move from procedure to follow-up with all required steps completed).
Operational analytics examples:
- Turnover Metrics: How long does it actually take to move a patient from the lab to a recovery bed?
- Identifying care transition issues: Look for where handoffs get stuck. This includes slow documentation and scheduling delays.
- Monitoring adherence to care pathways: Are teams following the standardized protocols for specific cardiac conditions (education, meds, follow-up booked)?
For a comprehensive foundation on how analytics drives performance across the cardiology care continuum, read our pillar guide on The Role of Data Analytics in Modern Cardiology Care Delivery.
What “Closed-Loop” Cardiology Workflows Look Like in Practice
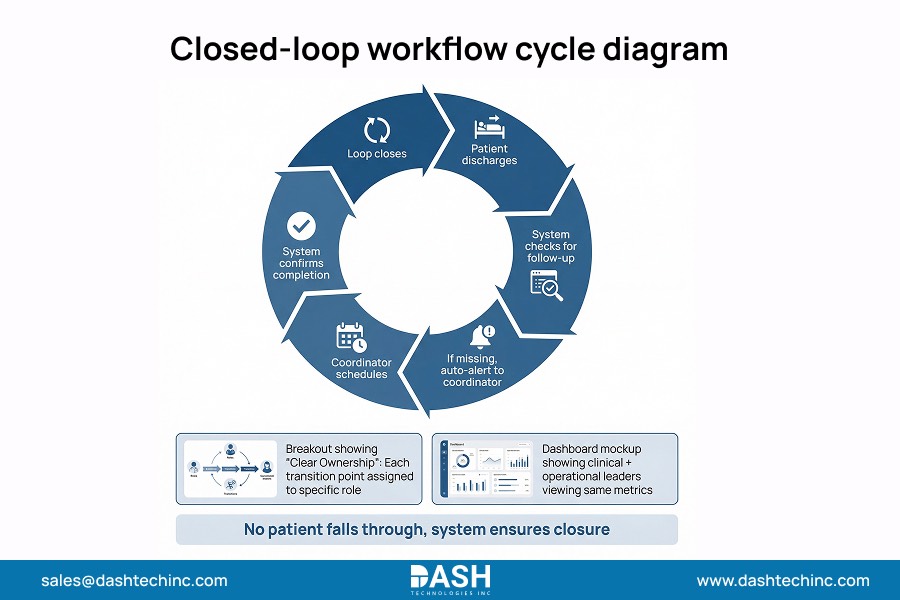
Closed-loop cardiology care means every transition has clear ownership, automated checks, and shared visibility. This is data-driven care coordination that ensures handoffs don’t rely on memory.
Automated alerts trigger for missed follow-ups. They activate when patients discharge without a scheduled appointment. Alerts also go off when scheduled appointments are unattended. Care coordinators get instant alerts. This helps them reach out proactively instead of finding gaps weeks later through readmission data.
Clear ownership at each transition establishes accountability. The system assigns specific team members responsibility for ensuring diagnostic results reach the cath lab, procedural summaries are transferred to inpatient teams, and discharge instructions include confirmed follow-up appointments. Tracking shows exactly who completed each handoff and when.
Visibility for both clinical and operational leaders provides a shared understanding of workflow performance. Clinical directors see follow-up completion rates and readmission trends while operations managers track scheduling efficiency and resource utilization, both viewing the same underlying data driving coordinated improvement efforts.
This approach works because it creates accountability and visibility in system design. It doesn’t depend on individual vigilance, making it highly effective for cardiology workflow optimization.
Building a Data-Driven Cardiology Workflow Strategy
An effective cardiology workflow strategy needs clear planning. It should focus on technical integration and standardizing processes for healthcare data-driven workflows & cardiology workflow optimization.
- Step 1: Document the entire cardiac care journey from point of entry to follow-up care. List all steps along the way, including all systems, handoffs, and decision-making processes, to identify existing gaps.
- Step 2: Identify high-risk transition points where gaps most frequently occur. The discharge-to-follow-up transition typically ranks highest given its direct correlation with readmissions.
- Step 3: Connect key systems by linking cath lab platforms, EHRs, imaging systems, and scheduling software. Focus on the highest-risk gaps first
- Step 4: Use analytics to monitor continuity, tracking time between care phases and handoff completion rates rather than just volume.
Conclusion: Closing Data Gaps Is Essential to Modern Cardiology Care
Cardiology workflow optimization is increasingly about protecting the handoffs that protect patients and clinicians. Seamless workflows reduce delays, prevent redundant work, and build trust that “the system has it,” especially across the cath lab to follow-up transitions. Data continuity is foundational to improving cardiology care delivery because it supports better outcomes, better efficiency, and more sustainable teams.
For cardiology leaders looking to strengthen workflow continuity and improve care delivery, thoughtful integration and analytics strategies can make a measurable difference. If you’d like to discuss how your organization can close workflow gaps and build a more connected cardiology care model, Request a Strategy Discussion
Frequently Asked Questions
About Dash

Dash Technologies Inc.
We’re technology experts with a passion for bringing concepts to life. By leveraging a unique, consultative process and an agile development approach, we translate business challenges into technology solutions Get in touch.







